Transdermal patches offer a convenient way to deliver medications through the skin into the bloodstream. By adhering to clean, intact skin, these devices release a steady dose over hours or days, reducing the need for frequent oral dosing. Understanding how transdermal patches work reveals a transdermal drug delivery system that bypasses much of the digestive system and first-pass liver metabolism, improving consistency and reducing certain gastrointestinal side effects. This overview also covers types of transdermal patches and why their designs matter for reliable dosing. For practical context, the nicotine patch serves as a classic example of a transdermal delivery option and helps illustrate patch safety guidelines.
From a terminology perspective, you may encounter skin patches, percutaneous delivery devices, or cutaneous delivery systems that enable medicine to reach the bloodstream through the skin. These LSI-aligned terms connect related concepts such as topical patches, hormone patches, nicotine replacement therapies, and adhesive transdermal systems, helping readers recognize common product labels. Understanding this broader language supports better conversations with healthcare providers and more informed choices about patch-based therapies.
Transdermal patches: How They Work
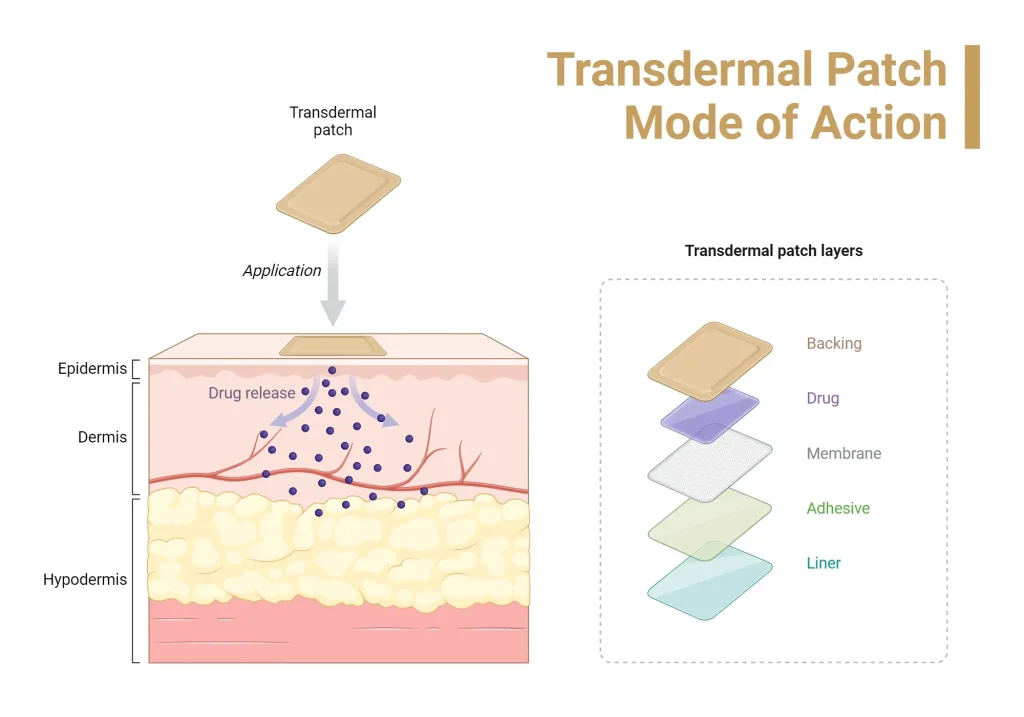
Transdermal patches deliver medicine by releasing drugs through the skin into the bloodstream, a process that relies on diffusion across the skin’s outer barrier. The basic patch design often includes a backing layer, a drug-containing layer, a rate-controlling membrane or adhesive matrix, and an adhesive that sticks to the skin. Together, these components enable a steady flow of medication over hours or days, illustrating the core concept of the transdermal drug delivery system.
Understanding how transdermal patches work involves considering factors such as drug diffusion, solubility, and the skin’s barrier properties. The drug’s molecular size and lipophilicity influence its ability to pass the stratum corneum, the skin’s outermost layer, and reach systemic circulation. When designed properly, a patch maintains a reliable release rate while minimizing irritation and variability in absorption.
Types of Transdermal Patches: DIA, Reservoir, Matrix, and Hormone Designs
The phrase types of transdermal patches describes several common configurations used to control drug delivery. Drug-in-adhesive (DIA) patches disperse the active ingredient directly within the adhesive that adheres the patch to the skin, making them simple and versatile for many medications, including nicotine patches.
Reservoir patches contain a drug-filled compartment separated from the skin by a rate-controlling membrane, which helps maintain a consistent dose. Matrix patches disperse the drug throughout a solid or semi-solid matrix, with diffusion through the matrix governing release. Hormone and specialty patches are tailored for stable, long-term dosing in therapies such as estradiol, testosterone, or other hormonal and neurological indications.
The Nicotine Patch: Dosing, Benefits, and Safety Considerations
The nicotine patch is a well-known example of a transdermal patch designed to aid smoking cessation. It delivers a controlled amount of nicotine over 16–24 hours or longer, depending on the product, helping reduce withdrawal symptoms and cravings while supporting a quit attempt or reduction in cigarette use.
When using a nicotine patch, careful dose planning is important. Programs often begin with a higher strength and gradually taper down. Clinicians may advise coordinating nicotine patches with other nicotine-containing products and monitor cardiovascular factors such as heart rate and blood pressure, since nicotine can influence these parameters in some individuals.
Transdermal Drug Delivery System: Principles, Pharmacokinetics, and Applications
A transdermal drug delivery system is designed to maintain therapeutic drug levels with controlled release through the skin. Key pharmacokinetic considerations include absorption rate, bioavailability, onset of action, and the duration of effect, all influenced by the patch’s design and placement.
This approach finds applications across domains such as pain management, cardiovascular therapy, and hormonal treatment. Innovations in rate-controlling membranes, adhesive matrices, and skin-permeation technologies continue to expand the potential payloads and patient-friendly dosing schedules within the transdermal drug delivery framework.
Patch Safety Guidelines: Best Practices for Safe Use
Patch safety guidelines emphasize careful skin care, site selection, and adherence to manufacturer instructions. Rotating application sites helps minimize irritation, and keeping the skin clean and dry before applying the patch supports consistent absorption.
Additional safety considerations include avoiding heat exposure that can increase drug absorption, not cutting patches, and proper disposal of used patches. Patients and caregivers should discuss potential drug interactions, contraindications, and special populations with a healthcare provider to ensure safe, individualized use.
Practical Guidance for Patients and Caregivers: Choosing, Applying, and Monitoring Patches
For patients and caregivers, selecting the right patch involves understanding the available designs (such as DIA, reservoir, and matrix types) and aligning them with the therapy’s dosing needs and lifestyle. Consulting healthcare professionals helps in choosing the appropriate patch, dosing schedule, and wear time.
Effective use also means applying the patch correctly, monitoring for signs of irritation or inefficacy, and maintaining a routine of site rotation and effect tracking. Clear instructions on reading labels, recording responses, and knowing when to seek medical advice support safer, more consistent outcomes with transdermal therapies.
Frequently Asked Questions
How do transdermal patches work?
Transdermal patches deliver the active drug from the patch through the skin into the bloodstream, providing a steady dose over hours or days. They consist of layers such as a backing, drug-containing layer, rate-controlling membrane or adhesive matrix, and an adhesive contact layer. The drug diffuses across the skin’s outer barrier into systemic circulation, with release rate influenced by patch design (drug-in-adhesive, reservoir, or matrix), skin condition, and temperature.
What are the types of transdermal patches?
The main types of transdermal patches include drug-in-adhesive (DIA) patches, reservoir patches with a rate-controlling membrane, and matrix patches where the drug is dispersed in a solid or semi-solid matrix. Hormone and specialty patches are designed for long-term dosing. Each type offers different release profiles and is chosen based on the drug’s properties and patient needs.
What is the nicotine patch and how should it be used?
The nicotine patch is a common transdermal patch used to support smoking cessation by delivering nicotine over 16–24 hours. It comes in strengths such as 21 mg, 14 mg, and 7 mg. Apply to clean, dry skin, rotate sites, press firmly for about 30 seconds, and wear as directed. Do not cut patches or expose them to excessive heat; monitor the patch site for irritation and discuss any cardiovascular concerns with a clinician.
What is the transdermal drug delivery system and its benefits?
A transdermal drug delivery system uses patches to move drugs through the skin into the bloodstream, bypassing the digestive system and first-pass liver metabolism. Benefits include steady drug levels, improved adherence due to longer wear times, and reduced gastrointestinal side effects. Not all drugs are suitable for this route, and patch design and skin tolerability influence effectiveness.
What are patch safety guidelines?
Patch safety guidelines cover skin preparation, site rotation, wear time, and disposal. Apply patches to clean, dry skin, rotate sites, and remove before activities that may affect adhesion; do not cut patches and follow disposal instructions. Avoid heat sources as heat can increase absorption. Be aware of potential skin reactions and drug interactions, and seek medical advice if irritation occurs or contraindications exist.
What factors affect the effectiveness of transdermal patches?
Absorption is influenced by skin condition and placement, ambient temperature, and patch integrity. Drug properties such as molecular weight and lipophilicity, along with patch design (DIA, reservoir, or matrix), determine release rate and skin uptake. Environmental factors and individual variability can also affect the delivered dose.
| Aspect | Key Points |
|---|---|
| What they are | Adhesive-backed devices that deliver drugs through the skin into the bloodstream for a steady, extended effect. |
| How they work | Layers include backing, drug-containing material, rate-controlling membrane or matrix, and an adhesive layer; the drug diffuses through skin into systemic circulation. |
| Key factors for effectiveness | Drug properties (molecular size, lipophilicity), patch design (reservoir, matrix, drug-in-adhesive), skin condition, temperature, and adhesion/duration. |
| Patch types | Drug-in-adhesive (DIA) patches; Reservoir patches; Matrix patches; Hormone and specialty patches. |
| Common uses | Nicotine patches for smoking cessation; pain-relief patches; hormone replacement patches; other systemic therapies (e.g., fentanyl, NSAIDs, antiemetics). |
| Safety and handling | Site rotation, wear times, avoid damaged skin, avoid excessive heat, monitor irritation, do not cut patches, proper disposal, discuss drug interactions and special populations. |
| Usage steps | Read label; prepare clean, dry skin; apply firmly; wear as directed; remove and dispose; rotate sites; monitor effects. |
| Nicotine patch specifics | Common strengths include 21 mg, 14 mg, 7 mg; reduces withdrawal and cravings; gradual dose reduction; consider cardiovascular factors; skin care and rotation. |
| Benefits and limitations | Benefits: steady drug levels, improved adherence, avoidance of first-pass metabolism. Limitations: not all drugs are suitable, skin reactions, variable absorption, cost/access. |
| Future trends | Matrix patches with enhanced permeability, microneedle patches, smart patches with wireless monitoring and dose adjustment; safety and regulatory oversight. |
Summary
Transdermal patches provide a meaningful approach to delivering medications with controlled, steady dosing for improved adherence and tolerability in suitable drugs, reflecting ongoing innovations in this delivery route.