Transdermal patches are transforming wound care by delivering medications through the skin in a convenient, non-invasive way. From easing pain to supporting skin healing, Transdermal patches enable steady, controlled release, a core idea in transdermal drug delivery and skin patch therapy. For wound care, these patches can be designed as a transdermal patch for wounds that minimizes gastrointestinal side effects while improving adherence. Understanding adhesive patch safety, potential irritation, and proper site selection helps patients maximize benefits and minimize risks. They come in various forms, with different types of transdermal patches tailored to drug type, dose, and duration of therapy.
From a semantic standpoint, these devices are topical delivery systems that push therapeutic compounds through the skin barrier. Alternative labels such as percutaneous drug delivery devices, skin-attached patches, or medicated tape reflect the same concept in different terms. LSI-friendly ideas include localized therapy, transcutaneous administration, and controlled-dose skin patches. Design considerations focus on adhesion, skin compatibility, and integration with wound care regimens. Together, these perspectives explain how such patches support healing while minimizing systemic exposure.
Transdermal Patches in Wound Care: Mechanisms, Benefits, and Practical Use
Transdermal patches are adhesive devices designed to deliver drugs across the skin. For wound care, they offer a non-invasive route to provide analgesia, anti-inflammatory therapy, or healing promoting agents, with steady dosing and reduced gastrointestinal impact. This approach aligns with transdermal drug delivery principles and supports safer, more predictable treatment outcomes.
The patch includes an adhesive matrix, a backing layer, and sometimes a rate-controlling membrane to regulate release. In practice, this design supports localized skin health while maintaining patient comfort and adherence. The approach benefits from skin patch therapy concepts, optimizing timing and site management to maximize therapeutic effect.
How Transdermal Drug Delivery Works for Skin Healing
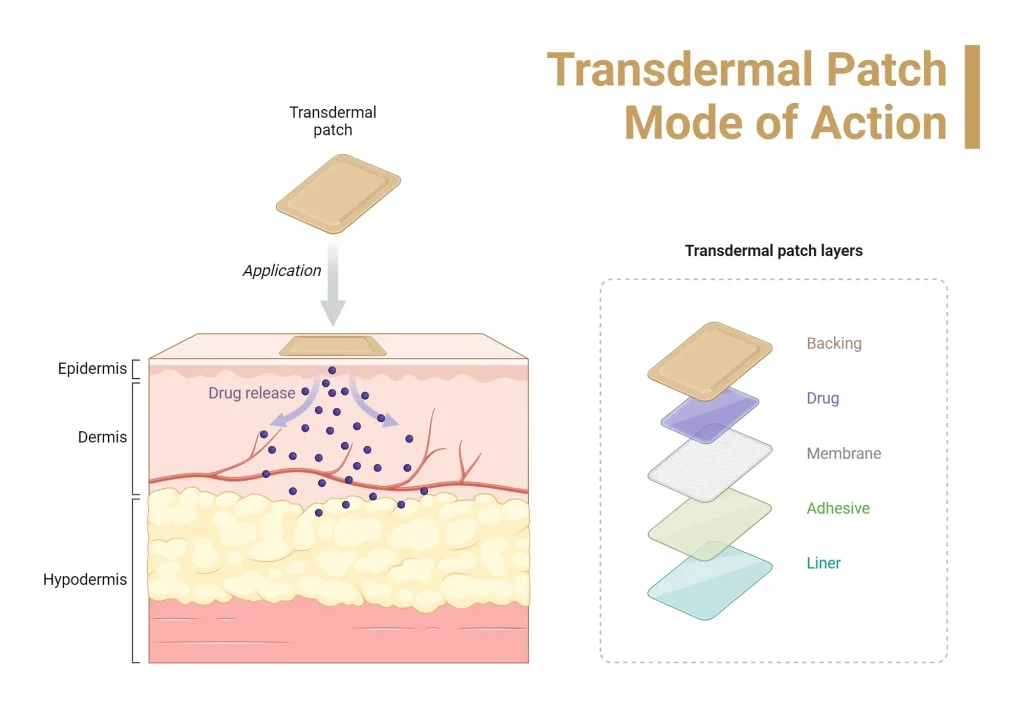
At the core, transdermal patches rely on a formulation that diffuses through the stratum corneum and into underlying tissues, delivering the active ingredient over hours or days. The layers—backing, adhesive reservoir or matrix, and protective liner—together govern release kinetics and bolster adhesive patch safety in clinical use.
This mechanism can support local action on wound beds or provide systemic effects, depending on the drug. For pain control or inflammation reduction in wounds, transdermal drug delivery can improve comfort during dressing changes and support healing, while minimizing first pass metabolism.
Transdermal Patch for Wounds: Applications, Benefits, and Safety
Applications include analgesic patches for pain management in acute or chronic wounds, anti inflammatory patches to reduce swelling, antibiotic containing designs for local infection control, and skin therapies that support regeneration. The transdermal patch for wounds can deliver analgesics and anti inflammatory agents directly at the site.
Safety considerations are essential: assess skin irritation, adhesive reactions, and proper site selection. Patch testing or gradual introduction can identify sensitivities, and clinicians should guide wear time, rotation, and interaction with moisturizers or wound dressings to preserve adhesive patch safety.
Types of Transdermal Patches and Their Suitability for Wound Care
Common types include reservoir patches, matrix patches, and drug-in-adhesive patches, each with distinct release mechanisms. Reservoir patches use a dedicated drug reservoir separated by a membrane to control diffusion, while matrix patches embed the drug in a polymer matrix for gradual release. These configurations affect suitability for wound applications. These are among the types of transdermal patches used in wound care.
Choosing among these depends on the drug’s properties, desired release profile, and the wound or skin condition. Factors like adhesion, skin irritation potential, and interaction with wound beds are critical. Clinicians evaluate these attributes to match a patch with the intended therapeutic goal.
Skin Patch Therapy: Practical Usage, Adherence, and Site Management
Skin patch therapy emphasizes patient-friendly delivery with simple application and limited systemic exposure. Practical steps include preparing the skin, ensuring clean, dry surfaces, and avoiding oils or lotions that reduce adhesion. Proper application promotes consistent dosing and patient comfort.
Adherence is improved with predictable wear times, site rotation, and clear labeling for patients and caregivers. Consider interactions with topical products or wound dressings that may affect patch performance, and plan for safe disposal once therapy ends.
Choosing, Testing, and Monitoring Transdermal Patches for Wound Care
Selecting the right patch requires collaboration with a healthcare professional who can weigh wound type, patient health, and potential drug interactions. Clear labeling and patient education help ensure correct usage, timing, and site maintenance within a broader wound care strategy.
Ongoing monitoring focuses on signs of skin irritation, patch adhesion, and clinical outcomes such as pain control and healing progression. If irritation or diminished effect occurs, clinicians may adjust the patch type, wear time, or switch to an alternative delivery method, all while prioritizing adhesive patch safety.
Frequently Asked Questions
Transdermal patches: What are they and how do they enable transdermal drug delivery for wounds?
Transdermal patches are adhesive devices that deliver drugs across the skin into underlying tissues or the bloodstream. They bypass the digestive system, allowing a steady, controlled release of the active ingredient over hours or days. For wound care, transdermal patches can provide pain relief, anti-inflammatory effects, antibiotics, or healing agents through the skin, aligning with the goals of transdermal drug delivery and skin patch therapy.
Transdermal patches in skin patch therapy for wound care: how are they used and what benefits do they offer?
They offer a non-invasive alternative to pills or injections, delivering drugs directly to the skin and nearby tissues. Depending on the active ingredient, patches can provide local wound relief, controlled systemic exposure, and improved adherence due to simple wear-time. This supports skin patch therapy by targeting symptoms like pain, inflammation, infection risk, or hydration needs with transdermal drug delivery while reducing gastrointestinal side effects.
Transdermal patches: what are the main types of transdermal patches and which type is most suitable for wounds?
The common types include reservoir patches, matrix patches, drug-in-adhesive patches, and single-layer or multilayer designs. Reservoir patches hold drug in a separate pocket with a rate-controlling membrane; matrix patches disperse the medication within a polymer matrix; drug-in-adhesive patches have medication mixed directly in the adhesive layer. For wound care, the choice depends on the drug’s properties and desired release: matrix or reservoir designs are often used for steady transdermal drug delivery, with careful attention to adhesion and skin compatibility to support effective transdermal patch therapy.
Transdermal patches and adhesive patch safety: what safety considerations should I know?
Adhesive patch safety involves monitoring skin irritation, allergy, and adhesion quality. Some people may experience redness, itching, or blistering; patch testing or gradual exposure can help. Choose appropriate sites away from broken skin, rotate areas to minimize irritation, and follow recommended wear time. Be mindful of interactions with wound dressings or moisturizers, and dispose of used patches per guidelines. Safety is essential in transdermal drug delivery to maximize benefit and minimize adverse effects.
Transdermal patches: how should I apply and care for a patch on wounds to maximize effectiveness?
Prepare clean, dry skin and apply to intact skin away from a wound bed unless advised otherwise. Press firmly to ensure good adhesion, and hold briefly to seal. Avoid lotions, oils, or heat sources near the patch. Monitor the site daily for irritation and replace the patch as prescribed. Rotate sites to prevent skin irritation, and follow wear-time and disposal instructions. Do not cut or modify patches unless directed by a clinician, as this can alter dose and safety.
Transdermal patches: what are common myths about their use for wounds, and what does evidence say?
Common myths include that patches are risky or a last resort. In reality, transdermal patches, when used correctly, can provide safe, effective, non-invasive drug delivery for wound care, with steady dosing and fewer gastrointestinal side effects. Ongoing innovation—such as microneedle-enhanced patches and smart patches that monitor healing—may offer more precise therapy, though patient selection and clinician guidance remain important.
| Topic | Key Points |
|---|---|
| Focus keyword | Core topic: Transdermal patches; used for non-invasive drug delivery through the skin; targets wound care and skin health audiences. |
| Related keywords | transdermal patch for wounds, skin patch therapy, transdermal drug delivery, adhesive patch safety, types of transdermal patches (listed in post) – shown as related terms to guide SEO and content scope. |
| Post title | Transdermal Patches: A User’s Guide to Wound Care Essentials |
| Meta description | Transdermal patches unlock non-invasive drug delivery for wounds and skin healing. Explore types, usage, and safety for effective wound care and skin health for patients. |
| What are transdermal patches | Adhesive devices that deliver drugs across the skin into the bloodstream or targeted tissue, bypassing the GI tract for steady, controlled release. |
| How they work | Multiple-layer structure: backing, adhesive matrix/reservoir, optional rate-controlling membrane, protective liner. Delivers active agents gradually and aims to minimize irritation and ensure good skin contact. |
| Applications in wound care and skin health | Pain management, anti-inflammatory therapy, antibiotic delivery, and localized skin therapies to support healing and skin health. |
| Benefits | Controlled, sustained delivery; non-invasive; targeted local or systemic effects; improved adherence; potential safety advantages by avoiding GI exposure. |
| Types of transdermal patches | Reservoir patches, matrix patches, drug-in-adhesive patches, and single-layer/multilayer designs; selection depends on drug properties, release profile, and wound/skin needs. |
| Safety considerations | Skin irritation/allergy, adhesive effects, proper site selection, wear time/dosing, interactions with other products, and considerations for pediatric, elderly, pregnant, or breastfeeding patients. |
| Practical tips | Prepare skin; apply to clean/dry skin; ensure adhesion; monitor for irritation; rotate sites; proper disposal. |
| Choosing the right patch | Collaborate with a healthcare professional; consider wound type, overall health, skin condition, interactions, and integration with dressings and system therapies; emphasize clear labeling and education. |
| Common myths and future directions | Patches are not inherently risky when used correctly; future directions include microneedle-enhanced, smart patches and multi-agent/digital health-enabled systems. |
| Conclusion (base content) | Patches for wounds and skin health, specifically transdermal patches, offer a versatile, patient-friendly approach to delivering medications and supporting healing with controlled, non-invasive mechanisms. |
Summary
Conclusion: Transdermal patches offer a versatile, patient-friendly approach to wound care and skin health, delivering medications through the skin with controlled, non-invasive dosing. By understanding patch types, safety considerations, and proper usage, patients and caregivers can maximize benefits while minimizing risks. The field continues to advance with smarter designs and integrated health monitoring to further enhance wound healing and skin health outcomes.